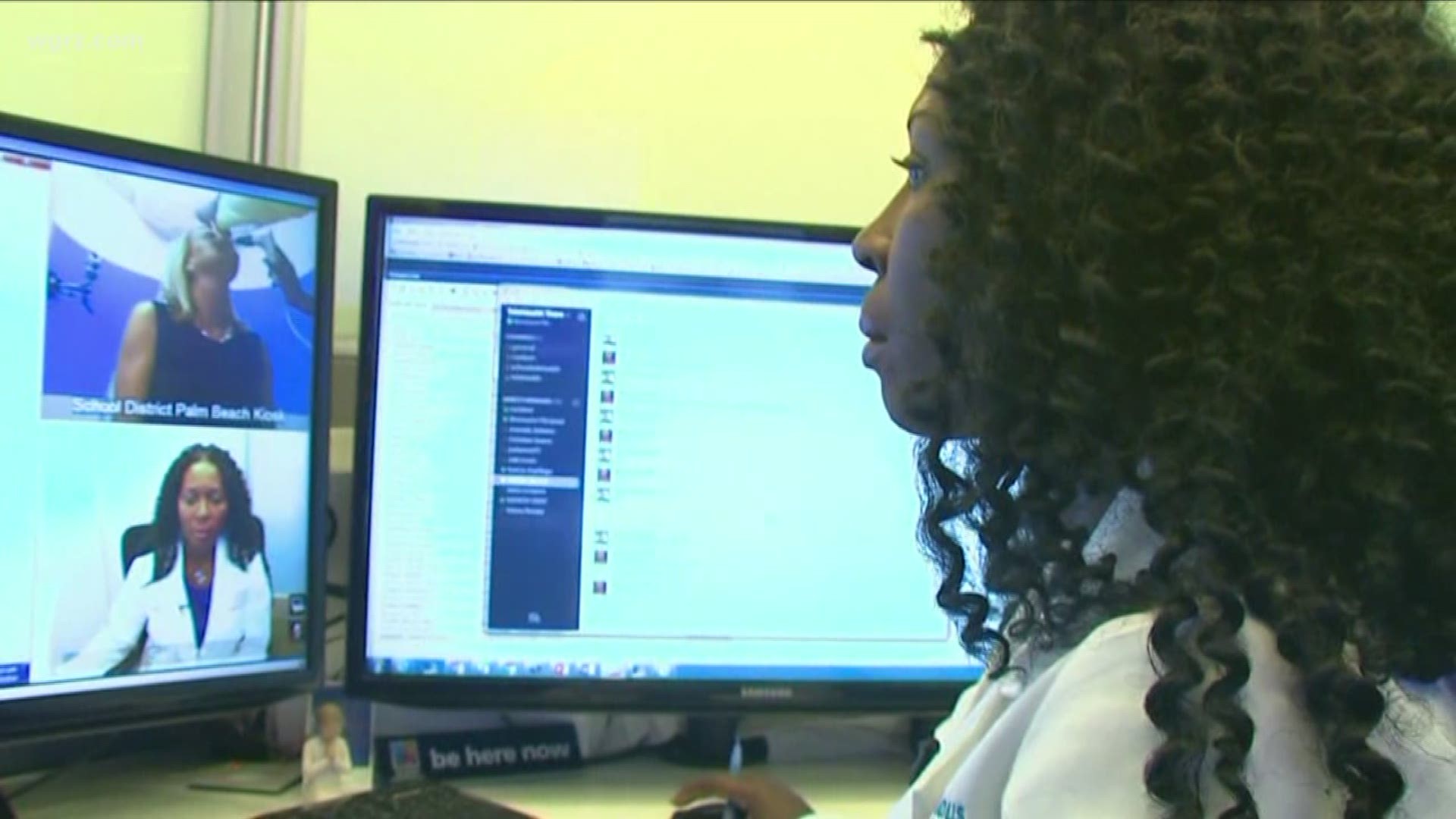
BUFFALO, N.Y. — Cough? Sniffles? Pink eye or strep throat? A growing number of patients are paying a "visit" to their doctor without leaving the comfort of their own home.
An appointment is as simple as a quick phone or video call, thanks to telemedicine technology. It gives patients greater access to health care providers — doctors, nurses, physician assistants, specialists, and even psychiatrists.
Telemedicine can be beneficial for people in rural areas, the elderly, those in drug treatment programs, or patients with developmental delays or physical limitations.
Telemedicine usage is up 53 percent, according to a 2019 J.D. Power study.
Buffalo-based Mobile Primary Care developed Mobile Telemed — software and technology that powers their virtual urgent care system. It's being used in patients' homes, schools, and nursing homes across New York State.
"We're managing patients in their own community, in their own residence to keep them at home to reduce costs and give them a higher quality of care," said Mobile Primary Care CEO Brian Egan.
A patient or nurse can initiate a video call and use bluetooth diagnostic equipment to check everything from temperature to heartbeat and pulse to the skin and ears.
"We have rapid response teams with mobile kits that actually go into the home, and they are able to dial up a practitioner after hours," Egan said.
A doctor on the other end of the telemedicine call can hear and see the results, make a diagnosis, and prescribe a treatment plan without being in the same room as the patient.

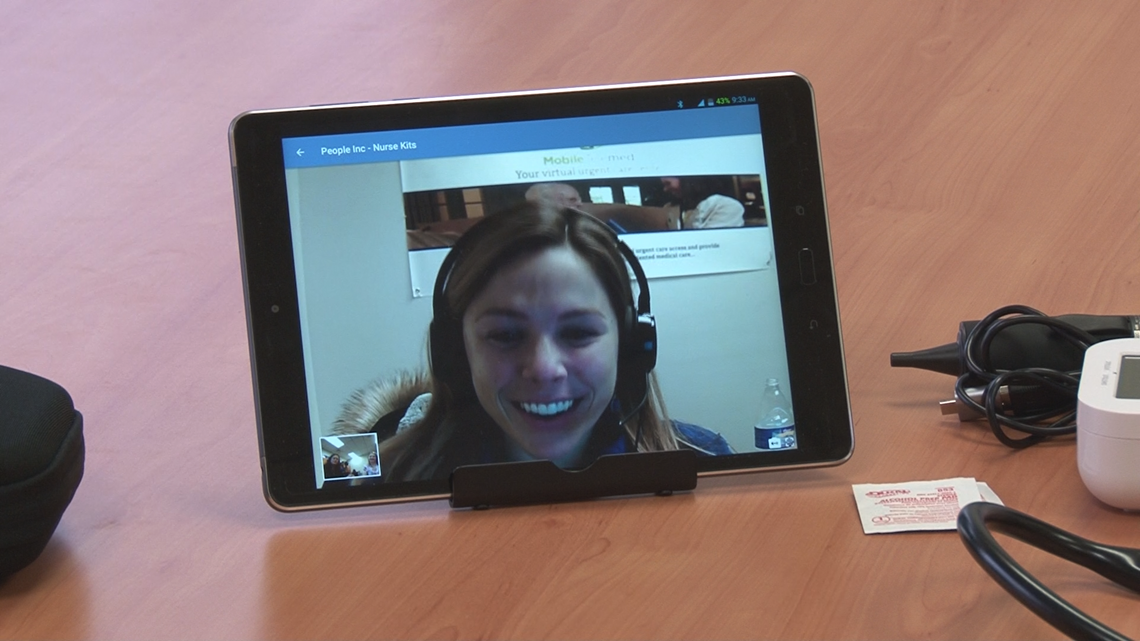
"We will walk through with the nurse doing the examination," said Dr. Ju Joh, associate chief medical officer at Mobile Primary Care. "We will ask the questions we normally do about what's going on with their health currently, what their chief complaint is and go through the whole history of present illness and previous medical history."
Mobile Primary Care has a team of more than two dozen doctors, nurses, and physician assistants.
The company provides telemed services for Genesee Valley Schools, the Frontier School District, and Salamanca City Schools.
Mobile Telemed also provides telepsych services where a patient can "visit" with a psychiatrist via video call.


Western New York's People Inc. is also using telemedicine.
The non-profit human services agency works with people with intellectual and developmental disabilities.
They adopted telemedicine in 2017 to treat people in their group homes. It's less stressful and cheaper than a trip to the emergency room.
"We know [individuals with developmental disabilities] go to the ER two to three times more than the average Medicaid patient," said Bonnie Sloma, senior vice president at People Inc. "We are able to use telemedicine as a tool to take care of people in place in our homes and provide a higher level of quality care at a lower cost."
In the case of People Inc., a staff member at the group home would first call People Inc.'s call center, and a nurse on the other end of the line determines if telemedicine is appropriate for that particular medical concern.
If telemedicine is a good fit, a nurse will then go to the home with equipment to do a virtual assessment and a video call with a doctor.


In 2018, People Inc. had 750 telemedicine visits and saw a 30 percent drop in emergency room visits.
"If it costs on average, transportation and staff costs $3,000 to go to an emergency room, and we can do it for less than $300 and treat in place? It makes economic sense to explore it and continue to build it out," Sloma said.
Eliminating an unnecessary trip to the emergency room also helps with the issue of lack of support staff in group homes. Normally a staff member has to travel with the patient to the hospital, so that takes away staff at the home.
People Inc. has been using telemedicine in Erie and Niagara Counties but recently started providing on-call and telemedicine services for people in Rochester.
They partner with different medical groups for procedures like X-rays and ultrasounds.
More insurance companies, such as Independent Health and BlueCross BlueShield of Western New York, are offering telemed benefits, from phone and video calls to app-based appointments.
Still there are barriers when it comes to telemedicine, such as insurance coverage and reimbursement or a lack of broadband access so patients, especially in rural areas, can connect virtually.
Dr. Andrew Talal from the Jacobs School of Medicine says telemedicine is a great way to treat people in underserved communities and those who are typically difficult to engage, such as those in substance abuse treatment programs.
Dr. Talal is leading a five year study on the use of telemedicine in drug treatment programs, specifically how it can help patients with Hepatitis C.


"The ability to engage those individuals in the places where they feel comfortable, I think really is the power and perhaps the next phase of development of this new modality of health care delivery," said Dr. Talal.
Dr. Talal said telemedicine allows for easier, more frequent followups with more privacy.
Francisco Humenyi is a Hepatitis C patient who is part of a substance abuse treatment program in Rochester. Dr. Talal is treating him even though the two have never met in person.
"We have two doctors on this, one that is in the room with me and one that I am talking to through a computer who will explain test results more in depth," Humenyi said. "I feel like that's all that's needed."